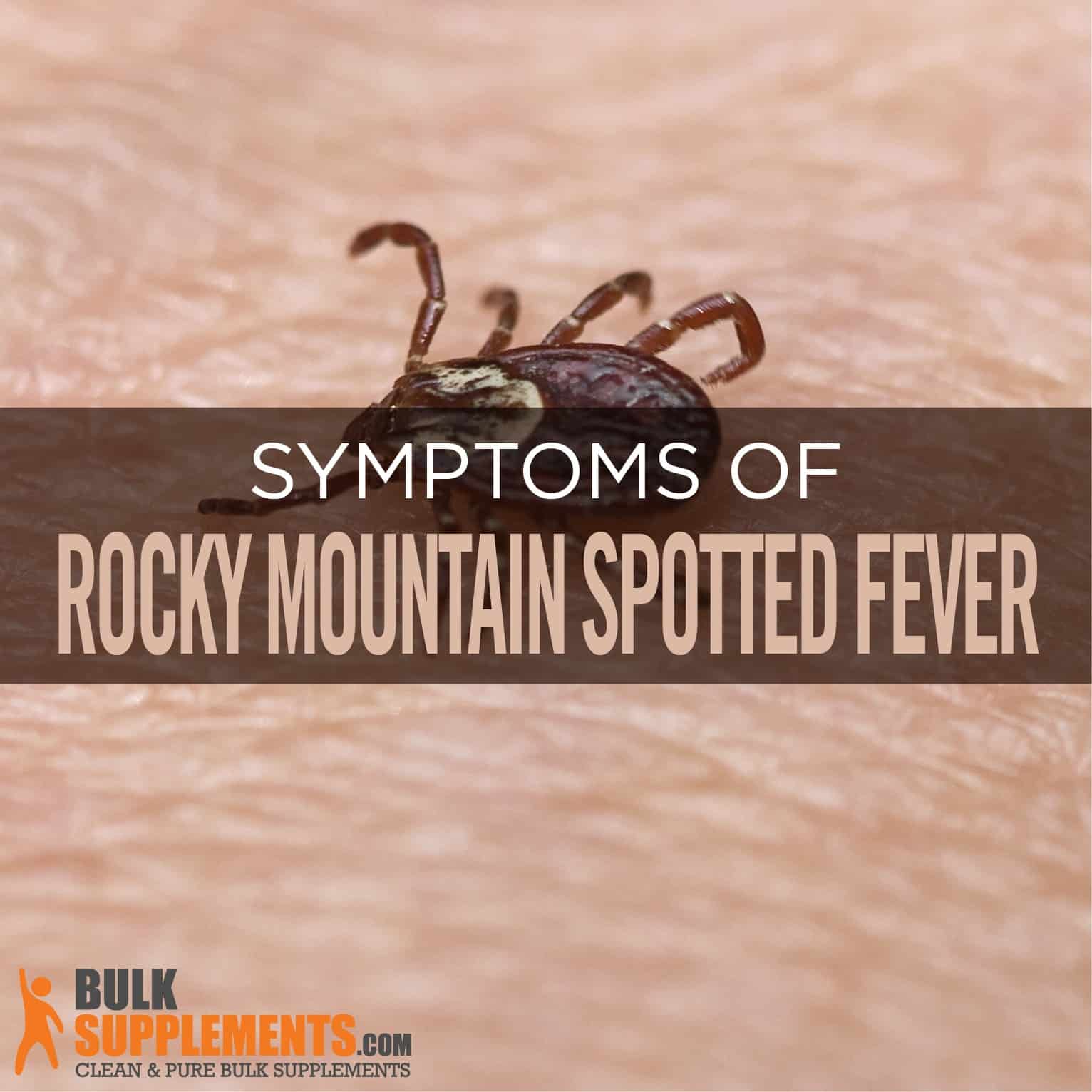
You’re looking at your arm and see a tiny, faint red dot. Maybe it’s a mosquito bite. Maybe you brushed against some brush while hiking. But then another appears. And another. If you've been searching for rocky mountain spotted fever images, you’re probably in that state of mid-afternoon panic where WebMD has convinced you that a tick bite is about to change your life.
Honestly? It might.
Rocky Mountain Spotted Fever (RMSF) is a bacterial infection spread by ticks, specifically Rickettsia rickettsii. It’s one of the deadliest tick-borne diseases in the Americas. The scary part isn't just the bacteria; it's how the symptoms masquerade as a common flu until things get really, really bad. If you wait for the "perfect" rash to appear before seeing a doctor, you might be waiting too long.
The rash is a liar. It doesn't always show up on day one. Sometimes it doesn't show up at all.
What Rocky Mountain Spotted Fever Images Don't Always Show You
When you scroll through medical databases, you see these vivid, angry purple spots. Those are the textbook cases. In reality, the early stages are subtle. Most people expect a bullseye like Lyme disease, but RMSF is a different beast entirely. It starts as small, flat, pink, non-itchy spots. They usually pop up on the wrists and ankles first. This is a huge diagnostic clue that many people miss because we tend to check our torsos or the bite site itself.
The bacteria actually attack the lining of your blood vessels. This is called vasculitis. Because the damage is happening to the "pipes" of your body, the rash is essentially blood leaking into the skin.
Early on, these spots blanch. That’s a fancy medical way of saying they turn white when you press on them. If you have a spot that disappears under your finger and then rushes back with color, that's an early-stage sign. Later, as the infection progresses and the blood vessel damage worsens, the spots become "petechial." They turn dark red or purple and no longer blanch. At that point, the "spotted" part of the name is incredibly obvious, but your internal organs are already under significant stress.
Roughly 10% of people with RMSF never develop a rash. That is a terrifying statistic. Doctors call this "spotless RMSF," and it’s actually more dangerous because it leads to delays in treatment. If you have a high fever, a crushing headache, and you were recently in a wooded area, don't wait for the skin to change.
The Timeline Matters More Than the Visuals
RMSF doesn't move at a leisurely pace. It’s fast.
Day 1 to 4: You feel like you have the worst flu of your life. High fever—often over 102°F. Chills. A headache that feels like a physical weight behind your eyes. Most people ignore this. They take some ibuprofen and go to bed.
Day 2 to 5: This is usually when the rash starts. It begins on the extremities. If you see spots on your palms or the soles of your feet, that is a massive red flag. Very few diseases cause rashes on the palms and soles.
If you aren't treated within the first five days of symptoms, the risk of permanent damage or death skyrockets. The CDC and experts like Dr. Christopher Paddock, a renowned rickettsiology researcher, emphasize that the antibiotic doxycycline is the gold standard. It needs to be started based on clinical suspicion, not a confirmed blood test. Why? Because the tests for RMSF usually come back negative in the first week. Your body hasn't made enough antibodies yet for the lab to see them, but the bacteria are already multiplying in your veins.
Why Location Changes Everything
We call it "Rocky Mountain" spotted fever, but that name is kind of a historical accident. It was first identified in the Rockies, but these days, it's way more common in the Southeast and parts of the Southwest. North Carolina, Tennessee, Missouri, Arkansas, and Oklahoma account for over 60% of cases.
And then there's Arizona.
In the last two decades, Arizona has seen a massive spike in RMSF carried by the brown dog tick. This is a big deal because the brown dog tick lives where people live—in houses and yards—rather than just in the deep woods. Images of RMSF in these regions often show more severe, rapid progression. In certain tribal nations in Arizona, the fatality rate has historically been much higher than the national average due to delayed access to care and high tick density.
Distinguishing RMSF From Other Rashes
It's easy to confuse RMSF with other issues. Here’s how to tell them apart without a medical degree, though you should still see a professional.
Lyme Disease: This usually presents as a single, expanding "bullseye" (erythema migrans). It’s usually not as "spotty" as RMSF.
Measles: Measles starts on the face and moves down. RMSF starts on the wrists/ankles and moves in toward the trunk. Plus, measles usually comes with a cough and runny nose (the "coryza").
Drug Allergies: These are often itchy and "hives-like." RMSF spots almost never itch. If you’re scratching the spots, it’s probably something else.
Menigococcemia: This is another deadly infection that causes a petechial rash. It’s hard to tell apart from late-stage RMSF visually. Both are medical emergencies.
The primary vector for RMSF in the eastern U.S. is the American dog tick (Dermacentor variabilis). In the West, it’s the Rocky Mountain wood tick (Dermacentor andersoni). These ticks are tough. They can go a long time without a meal. When they do find you, they need to be attached for several hours to transmit the bacteria, which gives you a window of opportunity to find them and pull them off.
Complications You Can't See in a Photo
If you look at rocky mountain spotted fever images and think, "Oh, it's just a skin thing," you’re missing the internal carnage. When the blood vessels leak, fluid moves into the lungs (pulmonary edema) and the brain (cerebral edema).
This leads to:
- Loss of circulation to fingers and toes, sometimes requiring amputation.
- Neurological deficits like hearing loss or paralysis.
- Kidney failure as the organs struggle with fluid balance.
There was a case study involving a young child who was initially misdiagnosed with a viral infection. By the time the rash appeared on her ankles, she was already in septic shock. This is why doctors are now trained to ask, "Have you been around ticks?" before they even look at the skin.
How to Protect Yourself and Your Family
Prevention is basically your only foolproof shield. You probably know about DEET, but permethrin is the real MVP. You spray it on your clothes, not your skin. It actually kills ticks on contact. If a tick crawls across your permethrin-treated hiking pants, it’s done for.
Tick checks are non-negotiable. Ticks love warm, dark places. Check the backs of knees, the groin, the armpits, and—most importantly—the scalp. Children are particularly prone to getting ticks in their hair.
If you find a tick, don't use a match. Don't use peppermint oil. Don't use nail polish. Those "hacks" just irritate the tick and make it more likely to vomit the bacteria into your bloodstream. Use fine-tipped tweezers. Grasp it as close to the skin as possible. Pull upward with steady, even pressure. If the head stays in, don't freak out. The bacteria are in the salivary glands and the gut, not the mouthparts. Just clean the area with alcohol and let the skin heal.
Treatment Realities
Doxycycline is the answer. Period.
There is an old myth that doxycycline shouldn't be given to children under eight because it can stain their permanent teeth. The CDC and the American Academy of Pediatrics have debunked this for short-term use in life-threatening cases like RMSF. The risk of the disease far outweighs the risk of cosmetic tooth staining. If a doctor hesitates to give a child doxycycline when RMSF is suspected, you need a second opinion immediately.
The recovery process can be long. If caught early, most people feel better within a few days of starting antibiotics. If treatment was delayed, the fatigue and muscle aches can linger for months. Some people even develop long-term vascular issues.
Actionable Steps for Suspected Exposure
If you have been in tick territory and start feeling "off," take these steps immediately. Do not wait for a rash to appear.
- Document the timeline. Write down when you were in the woods or when you found the tick. Note the exact day the fever started.
- Take photos. If a rash appears, take high-quality rocky mountain spotted fever images of your own skin. Use natural light. These are invaluable for doctors to track the progression (e.g., "Is it spreading toward the chest?").
- Seek "Doxy." When you go to the ER or urgent care, specifically mention your tick exposure. Use the words: "I am concerned about Rocky Mountain Spotted Fever."
- Monitor the "Spots." Check your palms and soles twice a day. This is a hallmark sign that separates RMSF from common viral exanthems.
- Check your pets. In many suburban cases, dogs bring the ticks inside. If your dog is lethargic or has a fever, they might have RMSF too. Talk to your vet about tick preventatives that actually work in your specific zip code.
The most important thing to remember is that you are the best advocate for your own health. Doctors see dozens of "fever and headache" cases every week during the summer. You are the one who knows you were pulling ticks off the dog or clearing brush in the backyard. That piece of information is more diagnostic than any blood test will be in those first critical 48 hours.
Stay vigilant, keep the tweezers handy, and never ignore a fever that comes with a headache after a day in the sun.